Medication Timing & Interaction Checker
Analysis Result
Recommended Safe Window:
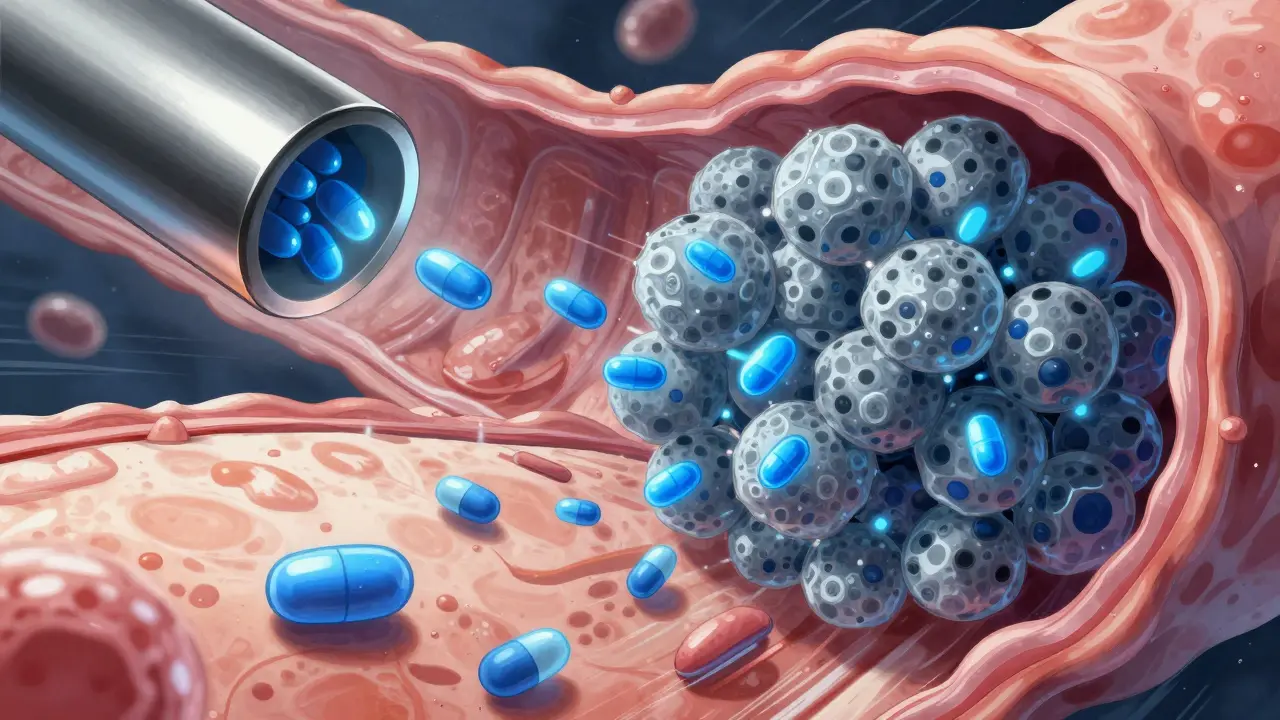
You've got a stubborn infection, and your doctor has prescribed a course of antibiotics. But you also have that familiar, burning feeling in your chest, so you reach for a quick-fix antacid. It seems harmless-one is for your lungs or skin, the other is just for your stomach. However, taking these two together can be a recipe for treatment failure. If you take an antacid at the same time as certain antibiotics, you could be accidentally blocking the medicine from ever reaching your bloodstream.
The problem isn't that the antacid "neutralizes" the antibiotic like a chemical reaction. Instead, it's a process called chelation. Some OTC antacids is non-prescription medications used to neutralize stomach acid and provide quick relief from heartburn and acid reflux. contain metal ions like aluminum, magnesium, or calcium. When these metals meet certain antibiotics in your gut, they act like a magnet, binding to the drug and forming a heavy, insoluble complex. This "clump" is too large for your intestinal wall to absorb, so the antibiotic simply passes through your system and ends up in the toilet rather than fighting your infection.
The Risk of Reduced Bioavailability
When we talk about "reduced absorption," we're talking about bioavailability-the amount of the drug that actually enters your circulation. For some patients, this interaction isn't just a minor dip; it's a crash. For example, Fluoroquinolones, a potent class of broad-spectrum antibiotics, are incredibly sensitive to this. If you take a drug like Ciprofloxacin with an aluminum-based antacid, your bioavailability can plummet from a healthy 70% down to a meager 15-25%. You're essentially giving yourself a fraction of the dose your doctor intended.
This creates a dangerous scenario. When the level of antibiotic in your blood drops below the "therapeutic threshold," the bacteria aren't fully killed. This doesn't just mean your infection lasts longer; it can actually train the bacteria to survive the drug, contributing to the global crisis of antibiotic resistance. In some clinical cases, patients with recurrent urinary tract infections have failed multiple rounds of treatment simply because they were taking calcium carbonate tablets, like Tums, too close to their medication.
| Antibiotic Type | Example Drug | Estimated Absorption Drop | Key Interacting Element |
|---|---|---|---|
| Tetracyclines | Doxycycline | 30% - 90% | Aluminum / Magnesium |
| Fluoroquinolones | Ciprofloxacin | 50% - 75% | Aluminum / Calcium |
| Penicillins | Amoxicillin | 18% - 22% | Aluminum-Magnesium |
Which Antacids Cause the Most Trouble?
Not all acid-reducers are created equal. The "classic" OTC antacids that provide immediate relief-those that work within 1 to 5 minutes-are usually the ones that cause the most interference. This is because they rely on metal salts to neutralize acid. Products like Maalox and Mylanta, which combine aluminum hydroxide and magnesium hydroxide, have a high binding capacity for antibiotic molecules.
If you look at your label and see aluminum hydroxide, magnesium hydroxide, or calcium carbonate, you're dealing with a high risk of chelation. These ingredients are effective at stopping heartburn, but they are essentially "glue" for certain antibiotics. On the flip side, if you can't avoid acid-reducing meds, you might consider options that don't use metal ions. H2-receptor antagonists (like famotidine) or Proton Pump Inhibitors (PPIs, like omeprazole) change the pH of your stomach without adding these binding metals, making them generally safer to use alongside antibiotics.
Mastering the Timing: The 2-to-4 Hour Rule
You don't necessarily have to choose between treating your infection and treating your heartburn; you just have to time it right. The goal is to ensure the antibiotic is absorbed into the bloodstream before the antacid arrives to block the door, or vice versa.
As a general rule of thumb, you should separate the two by at least 2 to 4 hours. However, the specific window depends on the drug class. For tetracyclines, a 2-hour gap is often the minimum. For the more sensitive fluoroquinolones, many medical guidelines suggest a wider gap-potentially 4 to 6 hours-to be completely safe. If you take your antibiotic at 8:00 AM, wait until at least 12:00 PM before taking an antacid. If you need the antacid first, wait several hours before taking your dose of antibiotics.
This isn't just a suggestion; it's a clinical necessity. Studies have shown that proper timing education can reduce treatment failure rates by nearly 28%. When the timing is off, you aren't just dealing with a stomach ache; you're risking a relapse of a systemic infection.

Practical Tips for Patients and Caregivers
Since only about a third of users are aware of these interactions, it's easy to miss the warning in the fine print. Here is a practical approach to managing your medications safely:
- Read the Label: Look for "Aluminum," "Magnesium," or "Calcium" in the active ingredients of your antacid. If you see them, be on high alert.
- Map Your Day: Use a phone alarm or a pill organizer to visualize the gap between your doses. Don't guess the time.
- Consult Your Pharmacist: Your pharmacist is the best resource for specific timing. Ask them, "Does this specific antacid bind with this specific antibiotic?"
- Consider Alternatives: If you have chronic acid reflux and are starting a long course of antibiotics, ask your doctor if a PPI or H2 blocker is a better temporary alternative.
Can I take Tums with my antibiotics?
Tums contain calcium carbonate, which can bind to certain antibiotics, particularly fluoroquinolones and tetracyclines, preventing them from being absorbed. You should generally avoid taking them at the same time. A gap of at least 2-4 hours is recommended to ensure the antibiotic remains effective.
Will any antacid stop my antibiotics from working?
Not all of them. The primary issue is with antacids containing metal ions (aluminum, magnesium, calcium). H2 blockers like famotidine or PPIs like omeprazole do not cause chelation, although they can still change stomach acidity, which might slightly affect the absorption of some drugs. Always check with your doctor.
What happens if I already took them together by mistake?
One accidental dose is unlikely to cause a total treatment failure, but doing it consistently throughout your course is a major problem. If you've done this repeatedly, contact your healthcare provider. They may need to adjust your dose or extend the treatment duration to ensure the infection is fully cleared.
Why does timing matter so much?
Timing matters because it prevents the antacid's metal ions from meeting the antibiotic in the stomach and intestines. By separating the doses, you allow the antibiotic to be absorbed into the blood before the antacid arrives, or you give the antacid time to leave the system before the antibiotic is introduced.
Are liquid antacids worse than tablets?
The form (liquid vs. tablet) is less important than the ingredients. Whether it is a chewable tablet or a liquid suspension, if it contains aluminum or magnesium hydroxide, it can trigger the chelation process and reduce the efficacy of your antibiotics.
Next Steps and Troubleshooting
If you are currently taking a course of antibiotics and experience severe heartburn, don't just reach for the first bottle in your medicine cabinet. First, check the antibiotic class. If you are on a "floxacin" (fluoroquinolone) or a "cycline" (tetracycline), the risk is highest. In this case, your first step should be to call your pharmacist to confirm the exact hour-gap required for your specific brand.
For those who struggle with chronic reflux, the best strategy is to move away from "on-demand" antacids during the antibiotic window. Switching to a daily PPI, under medical supervision, can keep the stomach environment stable without introducing the metal ions that block your medication. If you notice that your infection symptoms aren't improving despite taking your pills, mention your antacid use to your doctor immediately-it might be the missing piece of the puzzle.






Anna BB April 18, 2026
It's so wild how these little things can make such a huge difference in our health!!! I honestly never knew about the metal ions thing... just goes to show we really need to pay attention to the labels!!!!
Agatha Deo April 19, 2026
Oh, look at us, trusting the "fine print" and the pharmacists who are basically just corporate puppets. I'm sure the big pharma companies just love it when we "accidentally" reduce the efficacy of their drugs so they can sell us a second course of the same thing. How convenient for their profit margins, right? 🙄
Anmol Garg April 20, 2026
It's quite a humbling reminder that our bodies are complex chemical laboratories. We often rush through our recovery without considering the harmony of what we ingest, but taking a moment to align our timing is a small act of mindfulness that can lead to much better healing for everyone.
Randall Barker April 21, 2026
People are just fundamentally lazy. They can't be bothered to read a simple piece of paper provided by a medical professional, and then they wonder why they're contributing to the global antibiotic resistance crisis. It's a moral failure of the highest order to ignore these guidelines when the stakes are literally the survival of future medicine. If you can't manage a basic schedule for your pills, you have no business complaining about the healthcare system's failures.
Michael Lewis April 22, 2026
Exactly! Discipline is the only way this works. Set your alarms, map out your day, and stick to the plan. No excuses. If you want to get better, you have to actually follow the protocol to the letter!
Colleen Tankard April 23, 2026
The 2-to-4 hour gap is a total lifesaver! ✨ Love that we have options like PPIs if the heartburn is just too much to handle. Stay safe everyone! 🌸💖
Nathan Berlin April 25, 2026
Typical westerners needing a manual for everything 🙄’ just take the medicine and stop overthinking it 🇮🇳
Adele Shaw April 25, 2026
I can't even believe we live in a country where people don't know this basics. It's absolutely pathetic that our education system has failed so miserably that we have to post blogs about how to take a pill. My own doctor barely mentioned this and I had to fight just to get a clear answer. It's a disaster!
Rock Stone April 27, 2026
Just a heads up for anyone reading-don't stress too much if you missed a window once, but definitely try to tighten it up for the rest of the pack. We've all been there and it's totally fine as long as you adjust now. Keep pushing through the recovery!