Have you ever applied a cream to soothe a rash, only to find your skin burning and itching even worse hours later? It sounds counterintuitive, but this frustrating cycle is actually quite common. Many people assume that a reaction to a skin cream is just sensitivity, but it could be a genuine contact dermatitis caused by the medication itself. When the very treatment meant to heal becomes the trigger, identifying the culprit is the first step toward relief.
The Difference Between Irritation and Allergy
Not every red bump is an allergy. To manage the issue effectively, you need to distinguish between two main types of skin reactions. Irritant Contact DermatitisA non-immune-modulated irritation of the skin by a substance causing direct damage to the epidermal barrier happens when something harsh physically damages the skin's surface, like frequent hand washing or solvents. On the other hand, Allergic Contact DermatitisA delayed type IV hypersensitivity reaction that occurs upon reexposure to a specific allergen is an immune system response. This means your body remembers the substance and attacks it again next time you use it. While both look similar-red, itchy, swollen-the cause determines how you treat it.
Common Medications That Trigger Reactions
You might be surprised to learn that over 360 different drugs have been identified as potential skin allergens. The usual suspects aren't just prescription creams; sometimes, ingredients in OTC ointments are the problem. Antibiotics remain the leading cause. Specifically, NeomycinAn antibiotic found in many combination ointments that triggers allergic reactions in nearly 10% of patients tested appears in positive test results almost twice as often as others. Another common offender is bacitracin, often mixed with neomycin in popular household first-aid ointments. Even corticosteroids, used to treat inflammation, can cause their own version of allergy in about 1% of patients, creating a therapeutic paradox where the cure mimics the disease.
How Doctors Identify the Culprit
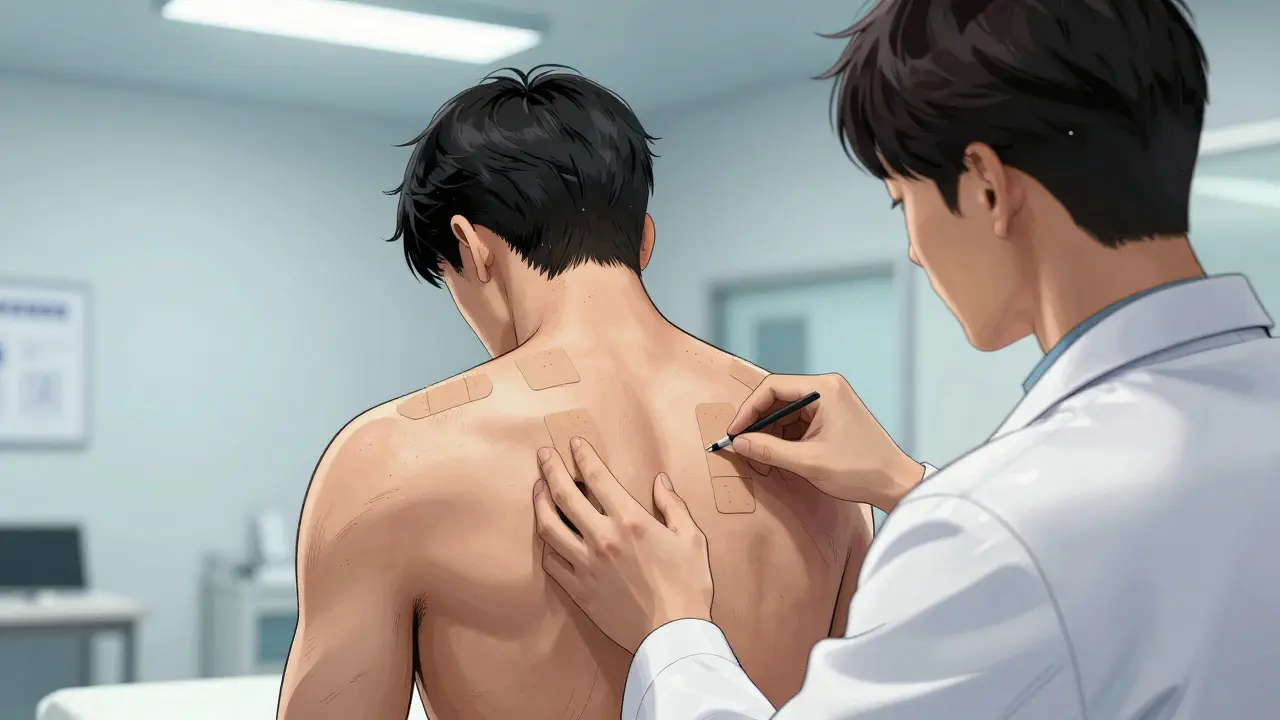
Guessing won't work here, especially if you have chronic issues. The gold standard for diagnosis is Patch TestingA methodology where suspected allergens are applied to the skin via adhesive patches for 48 hours to assess for delayed hypersensitivity reactions. During this procedure, small amounts of potential allergens are stuck to your back with tape. You wear them for 48 hours, avoiding water, and then return for readings at 48 and 96 hours. This slow reveal helps doctors confirm which specific chemical triggered your immune system. Recent improvements in the "Topical Medication Allergy Score" have made this diagnostic process significantly more accurate, helping identify causes in nearly 70% of suspected cases where previous methods failed.
| Substance Class | Specific Examples | Risk Factor |
|---|---|---|
| Antibiotics | Neomycin, Bacitracin, Gentamicin | Found in >90% of OTC antibiotic ointments |
| Preservatives | Methylisothiazolinone, Formaldehyde releasers | High risk in lotions and creams |
| Local Anesthetics | Benzocaine, Lidocaine | Common in numbing creams |
| Corticosteroids | Hydrocortisone, Clobetasol | Treatment itself can become the cause |
Effective Treatment Strategies
Once you know what hurts, the path to healing gets clearer. For mild localized cases, simple hydrocortisone is often the starting point. However, if the rash is widespread, stronger options are needed. High-potency Topical CorticosteroidsMid- or high-potency steroid medications like triamcinolone or clobetasol recommended as first-line therapy for severe lesions provide rapid symptom relief. There is a catch, though: they shouldn't stay on sensitive areas like eyelids or the face for too long, as they can thin the skin (atrophy).
If you cannot tolerate steroids, alternative classes exist. Non-steroidal options include topical calcineurin inhibitors such as TacrolimusA non-steroidal ointment that demonstrates 60-70% efficacy in managing allergic contact dermatitis symptoms (Protopic) and pimecrolimus (Elidel). These are often used on delicate skin. About 82% of patients report significant improvement within two weeks of switching to these medications, although some may experience a temporary burning sensation at the application site.

Living With a Diagnosis and Preventing Flare-Ups
Avoidance is the cornerstone of management. It's not just about skipping the prescribed cream; it's about reading labels on shampoos, detergents, and sunscreens. Hidden allergens lurk everywhere. One helpful tip is to bring your entire collection of skincare products to your appointment. Studies show that 30% of causative agents are actually found in non-prescription items that patients didn't consider "medications." Additionally, cross-reactivity is a real concern. If you react to one type of steroid, you might react to a group of them. Knowing your specific steroid group (A through F) helps doctors choose a safer alternative that won't trigger the same reaction.
Frequently Asked Questions
How long does it take for contact dermatitis to heal?
Complete resolution typically takes 2-4 weeks with appropriate treatment and strict avoidance of the trigger. However, itching often decreases significantly within the first 48 to 72 hours of starting therapy.
Can I use over-the-counter creams if I suspect an allergy?
Be cautious. OTC creams like hydrocortisone are good for mild irritation, but if your allergy is to preservatives found in those creams, they might worsen it. If symptoms persist after 7 days of OTC use, see a specialist.
Is patch testing painful or dangerous?
Patch testing is generally painless and safe. The substances are diluted to minimize risk. In rare cases, the test might cause a local flare, but serious systemic reactions are extremely uncommon under supervised conditions.






Rocky Pabillore April 1, 2026
People really struggle with basic skincare literacy. It is embarrassing how many skip reading labels before applying anything. Neomycin is common knowledge in my circle but seems like rocket science elsewhere. Stop blaming doctors for your own ignorance regarding ingredients. You should have checked the package insert first.
Molly O'Donnell April 3, 2026
Neomycin sensitivity is rampant yet ignored in standard protocols everywhere.
Owen Barnes April 3, 2026
That is indeed a valid point regarding clinical oversight. We shoulf acknowledge that preservatives play a huge roll too. Often people forget the vehicles in the cream matter just as much as the drug inside it. Education is key here though.
Callie Bartley April 3, 2026
Our healthcare system is so broken that we cannot even trust a simple ointment. This feels like another layer of corporate negligence pushed onto the patient. We pay taxes for better safety but get this garbage advice instead. It is absolutely infuriating to deal with these side effects alone.
Rod Farren April 4, 2026
The mechanism of delayed hypersensitivity is fascinating stuff! Type IV reactions involve T-cell mediated pathways which takes time to manifest. You cannot simply wash it off instantly because the immune memory persists in local tissues. Understanding the pharmacokinetics helps you manage expectations better. Stick with the patch test data over anecdotal reports!
Christopher Beeson April 5, 2026
Science is merely a tool for control rather than truth in this arena. They sell us solutions that create new problems in a never ending cycle. Your enthusiasm ignores the fundamental corruption of profit driven medicine. We are playing a game where losing hurts our bodies permanently. It is tragic that we rely on chemicals to fix damage from chemicals.
Arun Kumar April 6, 2026
I hope everyone finds relief soon because skin health impacts confidence greatly. Many of us share this struggle regardless of borders. The patience needed during healing is immense but worth it. Community support matters a lot during these difficult recovery phases. Keep pushing forward despite the confusion.
Eleanor Black April 6, 2026
I completely agree with your sentiment regarding community support.
It is truly heartbreaking when individuals feel isolated during such painful experiences.
The emotional toll often exceeds the physical discomfort involved.
Please know that many people here understand what you go through daily.
Recovery timelines vary significantly depending on individual physiology factors.
You should avoid scratching as much as possible to prevent scarring later.
Patience remains the most valuable resource in your arsenal right now.
Small improvements might seem insignificant initially but they add up over weeks.
Remember that your skin barrier needs rest and consistent care above all else.
Hydration plays a surprisingly large role in epithelial repair processes generally.
We should prioritize gentle cleansing methods without harsh surfactants nearby.
Listening to your body signals is paramount for avoiding future flare-ups entirely.
Please consult specialists who specialize in contact dermatology specifically.
Their expertise provides clarity that generalists might overlook sadly.
Stay strong through this difficult journey towards wellness again.
❤️🙏✨
Jenny Gardner April 8, 2026
This topic is incredibly important for public awareness!
Safety standards must improve dramatically across the board!!!
Reading labels is non-negotiable now!!
Avoid hidden allergens wherever you can!!!!
It is vital for self-protection against chemical triggers!!!!!
Sharon Munger April 9, 2026
agreed on the label reading part sometimes the ingredients lists are hard to decipher but we have to try
nice tips thanks for sharing
we all learn from these mistakes
James DeZego April 10, 2026
Good info on patch testing methods there 👍 Everyone knows cross reactivity is sneaky. Steroid groups matter a lot in switching meds 💡 Always check group A through F classifications. Stay safe out there friends 🛡️
Cara Duncan April 10, 2026
Sending love to anyone dealing with rashes currently 🌸 Healing takes time but you will get there 😊 Don't stress too much about perfection 🧖♀️ Just take it one day at a time 💕 You deserve gentle care always ✨
Russel Sarong April 11, 2026
Such beautiful words!!! Every single person deserves kindness like this!!!! You are spreading positivity!! This is exactly what the community needs!!! The emotional impact is real!!!! Thank you for being so compassionate!!!