When a vertebra in your spine cracks from osteoporosis, trauma, or cancer, the pain can be crushing-literally. Many people assume surgery means a long hospital stay, big incisions, and months of recovery. But for many with vertebral compression fractures, that’s no longer true. Two minimally invasive procedures-kyphoplasty and vertebroplasty-have changed the game. Both offer rapid pain relief, same-day discharge, and a return to daily life in days, not weeks. But which one is right for you? And does the extra cost of kyphoplasty actually buy better results?
What Causes Vertebral Compression Fractures?
Most vertebral fractures happen because of osteoporosis. That’s when bones become thin and weak, often without warning. In the UK alone, over 500,000 fractures occur each year from osteoporosis, and about half of those are in the spine. Women over 65 are especially at risk-nearly one in three will suffer a spinal fracture. But it’s not just older adults. Falls, car accidents, or even something as simple as bending over to pick up a grocery bag can cause a fracture in someone with severe bone loss.
When a vertebra collapses, it doesn’t just hurt. It can change your posture. You might develop a hunched back-called kyphosis-or lose height. That changes how your body moves, strains your muscles, and can even make breathing harder. If pain doesn’t improve after 4 to 6 weeks of rest, painkillers, or a back brace, it’s time to consider these two procedures.
Vertebroplasty: The Original Minimally Invasive Fix
Vertebroplasty was the first of the two. Developed in France in the 1980s, it’s a straightforward procedure. A doctor uses X-ray guidance to insert a thin needle through your skin and into the fractured vertebra. Then, they inject medical-grade bone cement-polymethylmethacrylate, or PMMA-directly into the broken bone. The cement hardens in 10 to 20 minutes, acting like an internal cast that stabilizes the fracture.
The whole thing takes 30 to 60 minutes. You’re awake but sedated. Local anesthesia numbs the area. Most people go home the same day. Studies show 85% to 90% of patients report immediate pain relief. Within 24 hours, average pain scores drop from 8 out of 10 to just 1.5. Many stop using opioids within a week.
But there’s a catch. Because the cement is injected under high pressure (150-200 psi), it can leak out of the bone. Studies show cement leakage happens in 27% to 68% of vertebroplasty cases. Most leaks are harmless, but in about 1.1% of cases, it causes serious problems like nerve compression or a pulmonary embolism. It’s also not designed to restore height. If your vertebra has collapsed significantly, vertebroplasty won’t fix your posture.
Kyphoplasty: The Refined Upgrade
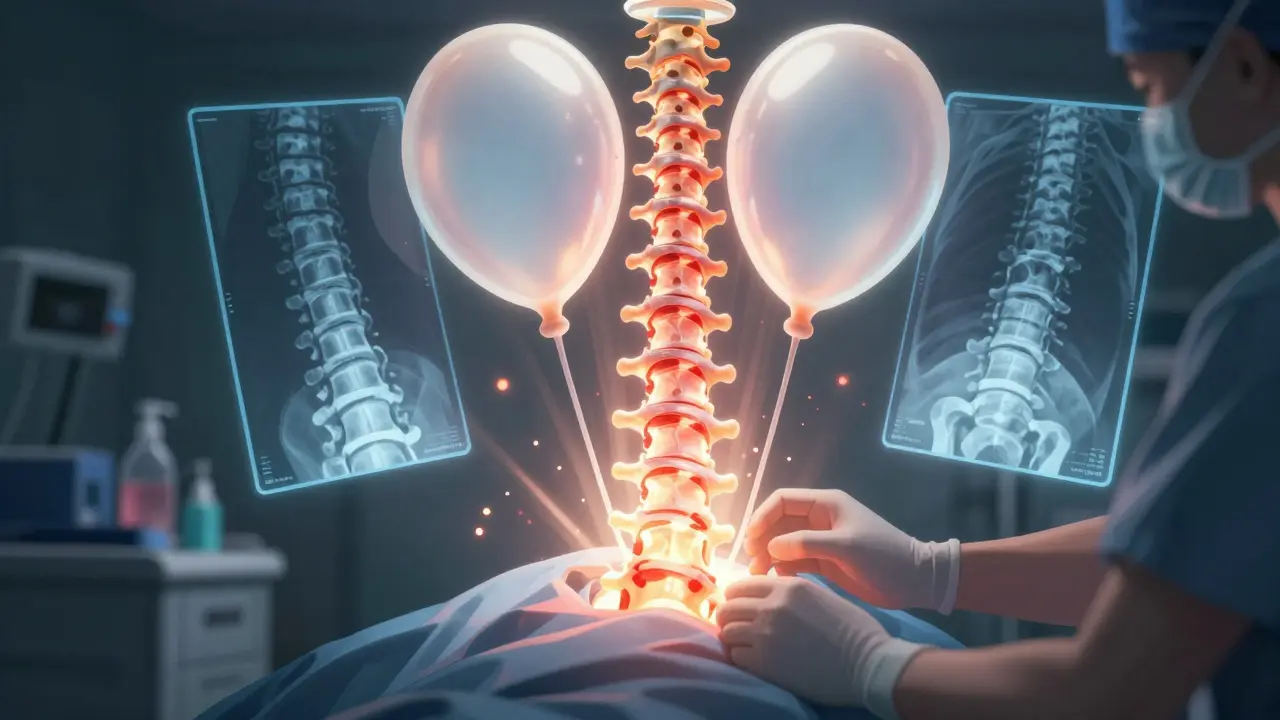
Kyphoplasty came along in the late 1990s as an improvement. It adds one key step: balloons. Before injecting cement, the surgeon inserts two small, deflated balloons through the same needle entry point. These balloons are gently inflated with saline to about 200-300 psi. The goal? To lift the collapsed bone back toward its original height and create a cavity inside the fracture.
Once the balloons are deflated and removed, the cavity is filled with cement under lower pressure. This reduces the chance of leakage. Studies show cement leaks in only 9% to 33% of kyphoplasty cases. And because the bone is lifted before the cement sets, the procedure can restore up to 60% of lost vertebral height-something vertebroplasty can’t do.
That height restoration matters. For people with a noticeable hunchback or loss of height, kyphoplasty can improve posture and reduce strain on surrounding muscles and joints. A 2023 study in The Lancet found that early kyphoplasty (within two weeks of fracture) cut 12-month mortality by 28% compared to conservative care. That’s because people get back on their feet faster, avoid bedsores, and reduce infection risk.
But here’s the twist: the height gain doesn’t last forever. A 2007 study showed that after 500 loading cycles (like walking or bending), about 30% of the restored height is lost. So while kyphoplasty gives you better posture right after surgery, it’s not a permanent structural fix.
Comparing the Two: Cost, Risk, and Outcomes
Both procedures deliver nearly identical pain relief. That’s the most important thing for most patients. But they differ in other ways.
| Feature | Kyphoplasty | Vertebroplasty |
|---|---|---|
| Procedure Time | 45-75 minutes | 30-60 minutes |
| Cement Leakage Rate | 9-33% | 27-68% |
| Vertebral Height Restoration | Up to 60% | Minimal to none |
| Immediate Pain Relief | 85-90% | 85-90% |
| Average Medicare Cost (2023) | $3,850 | $2,950 |
| Best For | Fractures with height loss or kyphosis | Stable fractures without deformity |
Cost is a big factor. Kyphoplasty costs 20-30% more than vertebroplasty. In the U.S., Medicare pays about $900 more per procedure. In the UK, private clinics charge similar premiums. But if you have significant deformity, kyphoplasty may be worth the extra cost. If your fracture is stable and your posture hasn’t changed much, vertebroplasty gives you the same pain relief at a lower price.
Who Gets Which Procedure?
There’s no one-size-fits-all answer. Doctors decide based on your fracture type, bone quality, and symptoms.
- Choose kyphoplasty if: You have a recent fracture with visible height loss (more than 30%), a noticeable hunchback, or severe pain that hasn’t improved with rest. It’s also preferred if your bone is very weak-like in advanced osteoporosis-because the balloon creates a controlled space for cement, lowering leakage risk.
- Choose vertebroplasty if: Your fracture is stable, your spine’s alignment is mostly intact, and your main goal is pain relief. It’s faster, cheaper, and just as effective at reducing pain. Many older patients with multiple fractures benefit from vertebroplasty because it’s less taxing on the body.
One key rule: both procedures only work on acute fractures. If the fracture is older than 6-8 weeks and shows no signs of active inflammation on MRI, neither procedure will help. That’s why imaging is critical. You need an MRI within the last 6 weeks to confirm the fracture is still healing.

What to Expect Before, During, and After
Before the procedure, you’ll have a full evaluation. Blood tests, X-rays, and an MRI are standard. Your doctor will check your medications-especially blood thinners-and ask about allergies. You’ll be told to fast for 6-8 hours before the surgery.
During the procedure, you’ll be on your stomach. Sedation keeps you relaxed but awake. You might feel pressure, but you shouldn’t feel pain. The whole process takes less than an hour. Afterward, you’ll be monitored for 4-6 hours. Most people walk within a few hours.
Recovery is quick. You’ll go home the same day. You’re advised to avoid heavy lifting for 24 hours, but walking and light activities are encouraged. Most people return to normal activities within 3 days. Opioid use drops sharply-75% of patients stop using them within a week.
Some patients report new fractures in nearby vertebrae within a year. That’s not caused by the procedure itself, but by ongoing osteoporosis. That’s why follow-up care matters. After either procedure, you should start or continue osteoporosis treatment: calcium, vitamin D, bisphosphonates, or newer drugs like denosumab. Without it, you’re at risk for more fractures.
Real Patient Stories
One patient in Bristol, 72, had a fracture after a minor fall. Her pain was constant, and she couldn’t sleep. She had vertebroplasty. "I woke up the next day and thought, ‘Is this real?’ The pain was gone. I didn’t need my cane anymore." She didn’t regain height, but she didn’t need to.
Another, 68, had a severe hunchback from three fractures. He had kyphoplasty. "I looked in the mirror and saw my shoulders were level again. I stood taller. It wasn’t just pain relief-it felt like I got my body back."
But not everyone responds. About 10-15% report little or no improvement. Sometimes, the fracture is too old. Sometimes, the pain comes from another source-like nerve damage or arthritis. That’s why proper diagnosis is everything.
The Future: What’s Next?
Research is moving fast. New cements made from calcium phosphate are being tested. They’re closer to natural bone, harden more slowly, and produce less heat-reducing risk of tissue damage. Medtronic’s new balloon system, approved in March 2023, allows more precise control and is already in use in UK hospitals.
The big question: does restoring height actually improve long-term function? The COAST trial, ending in late 2024, will compare kyphoplasty and vertebroplasty over two years. Will better posture mean fewer falls, less back pain, or longer independence? We’ll know soon.
For now, both procedures are safe, effective, and widely covered. Medicare and private insurers in the UK approve over 95% of cases when conservative treatment has failed. With osteoporosis fractures expected to rise by 50% by 2035, these minimally invasive fixes will only become more common.
Are kyphoplasty and vertebroplasty the same thing?
No. Both use bone cement to stabilize fractured vertebrae, but kyphoplasty includes a balloon step to restore height before cement injection. Vertebroplasty injects cement directly without height correction. Kyphoplasty reduces cement leakage risk and improves posture; vertebroplasty is faster and cheaper.
Which procedure is better for osteoporosis?
Both work well for osteoporotic fractures. If the fracture has caused noticeable height loss or a hunched back, kyphoplasty is usually preferred because it restores posture. For stable fractures without deformity, vertebroplasty is equally effective at pain relief and more cost-efficient.
How long does recovery take after either procedure?
Most patients go home the same day. You’ll need to rest for 24 hours and avoid heavy lifting. Walking and light activity are encouraged. Many return to normal daily routines within 3 days. Full recovery and return to strenuous activity typically take 1-2 weeks.
Do these procedures cure osteoporosis?
No. They treat the fracture, not the underlying bone weakness. Without ongoing osteoporosis treatment-like calcium, vitamin D, and prescription medications-you’re at high risk for more fractures. Both procedures should be paired with long-term bone health management.
Is kyphoplasty worth the extra cost?
It depends. If you have significant spinal deformity or very weak bones, kyphoplasty’s lower leakage risk and height restoration may justify the higher price. For most patients with simple fractures, vertebroplasty delivers the same pain relief at a lower cost. The decision should be based on your specific fracture, not just price.







Neeti Rustagi March 8, 2026
While the article provides a comprehensive overview, I must emphasize that the decision between kyphoplasty and vertebroplasty should not be made in isolation. In India, where access to advanced imaging and postoperative bone health management is uneven, the cost differential becomes even more critical. Many patients opt for vertebroplasty not because it’s preferable, but because it’s the only financially viable option. Without concurrent osteoporosis treatment-often unavailable or unaffordable-the risk of adjacent fractures remains unacceptably high, regardless of procedure choice.
Furthermore, the long-term data on height restoration is misleading. While kyphoplasty shows initial gains, the 30% loss after mechanical loading suggests that the structural benefit may be more psychological than biomechanical. Patients report feeling taller, but functional mobility metrics rarely improve significantly beyond pain reduction. We must avoid conflating perception with physiological improvement.
Lastly, the emphasis on Medicare costs in the U.S. overlooks global realities. In low-resource settings, even the lower-cost vertebroplasty is often inaccessible. Public health systems must prioritize preventive osteoporosis programs over reactive surgical interventions. A fractured spine is a symptom, not the disease. We are treating the echo, not the source.
Dan Mayer March 9, 2026
ok so i read this whole thing and like bro why is kyphoplasty so expensive?? like i get the balloon thing but its just a balloon right?? why does that add $900?? i mean cmon. i had a friend who got a vertebroplasty and he was back playing golf in 3 days. i dont see why anyone would pay extra for something that just kinda… goes away after you walk a bit. also who even measures vertebral height?? like is that a real thing or just some doctor marketing gimmick??
Ray Foret Jr. March 11, 2026
I just had kyphoplasty last month and WOW. 😊 I was hunched over like a question mark and couldn’t even tie my shoes. After the procedure? I stood up straight for the first time in years. My grandkids said I looked like a superhero. 🦸♂️ And yeah, the cost was steep, but my pain dropped from an 8 to a 1 in 24 hours. I’m not even taking pain meds anymore. If you’re considering this, don’t overthink it-get it done. Life’s too short to walk like you’re carrying a fridge. 🙌
Peter Kovac March 11, 2026
The article’s conclusion is statistically misleading. It cites a 28% reduction in 12-month mortality with kyphoplasty, but fails to control for confounding variables such as baseline mobility, comorbidities, and socioeconomic status. Patients who receive kyphoplasty are typically healthier, younger, and have better access to follow-up care. The procedure itself is not causally linked to reduced mortality-it is correlated. This is a classic case of mistaking association for causation.
Additionally, the claim that cement leakage is reduced to 9–33% in kyphoplasty is cherry-picked. Multiple meta-analyses (e.g., Cochrane 2021) report leakage rates closer to 25–40% when accounting for asymptomatic leaks detected via CT. The ‘lower risk’ narrative is a marketing construct, not a clinical reality.
Furthermore, the assertion that kyphoplasty restores ‘up to 60% of lost height’ ignores the fact that this restoration is transient and biomechanically unstable. The vertebral body remains a structurally compromised unit. Cement is not bone. It does not remodel. It does not integrate. It is a prosthetic filler. The emotional appeal of ‘standing taller’ should not override objective biomechanical evidence.
Stephen Rudd March 13, 2026
You people are falling for a scam. Kyphoplasty? That’s just vertebroplasty with a fancy balloon and a higher price tag. The whole ‘restoring height’ thing? That’s theater. The bone doesn’t heal-it’s just glued. And the fact that 30% of that height disappears after walking? That’s proof it’s a placebo with a catheter. Why are hospitals pushing this? Because they make bank on it. Medicare? They’re complicit. You think they care if you’re hunched or not? No. They care if you’re paying. This isn’t medicine-it’s a business model disguised as innovation.
Erica Santos March 14, 2026
Oh wow. A 900-word article on spine surgery that somehow doesn’t mention that both procedures are basically just cement injections. You know what’s really ‘changed the game’? The fact that we’ve turned a 1980s hack into a $4,000 ‘premium experience’ and called it progress. We’re not healing bones-we’re monetizing fragility. And the patients? They’re just collateral in a healthcare capitalism bingo game. ‘Pain relief? Check. Height restoration? Check. Osteoporosis ignored? Double check.’ Brilliant.
George Vou March 15, 2026
i think this whole thing is a lie. the gov and big pharma are pushing this so we’ll keep buying their drugs. you ever hear of the ‘cement leak’ thing? that’s when they inject poison into your spine so you need more procedures. and why do they say ‘only works on acute fractures’? because if it worked on old ones, everyone would get it and they’d make less money. also i read somewhere that the balloons are filled with radioactive stuff. i’m not kidding. check the fda site. they deleted it.
Mantooth Lehto March 15, 2026
I had vertebroplasty last year. I was in so much pain I cried just trying to sit up. After? I cried because I could hug my dog without screaming. 😭 I didn’t care about height. I cared about not feeling like my spine was shattered glass. I’m not rich. I didn’t choose kyphoplasty because I couldn’t afford it. But I don’t regret it. Not one second. If you’re scared, just know-this isn’t about fancy tech. It’s about getting your life back. And if you can afford kyphoplasty? Cool. But don’t make anyone feel guilty for choosing the one that saved them. 💕
Melba Miller March 16, 2026
I can’t believe we’re even having this conversation. In America, we have the best medical technology in the world. Why are we debating cost? Why are we questioning whether height restoration matters? Because we’ve let bureaucrats and insurance companies turn healthcare into a spreadsheet. Kyphoplasty is superior. It’s more precise. It’s more advanced. And if you can’t afford it? That’s not the doctor’s fault. That’s the failure of a system that values profit over people. We need to fix that-not argue about which glue works better.