Food Allergy Cross-Reactivity Checker
How This Works
Select your primary pollen allergy to see common foods that may cause cross-reactions (Oral Allergy Syndrome). This tool helps identify potential triggers that could worsen year-round allergy symptoms.
Key Takeaways
- Food allergies can keep your immune system on high alert, worsening seasonal or indoor allergies all year.
- Cross‑reactivity, especially between certain fruits and pollen, explains why symptoms overlap.
- Managing both food and environmental triggers together reduces overall allergy burden.
- Testing for specific IgE antibodies helps pinpoint linked allergens.
- Gut health and proper barrier function play a surprising role in allergic reactions.
When you hear the term Food allergies are immune‑mediated reactions that occur shortly after eating a specific food, you probably picture a single bite of peanuts causing swelling. But for many people, that reaction isn’t isolated-it can keep the immune system primed, making you sneeze, itch, or wheeze whenever you step outside, even in winter. That’s the core link between food allergies and year-round allergies.
What Exactly Is a Food Allergy?
A food allergy is an IgE‑mediated immune response where the body produces immunoglobulinE antibodies that recognize a food protein as a threat. Upon re‑exposure, those antibodies trigger mast cells to release histamine a chemical that causes itching, swelling, and airway constriction. The classic symptoms-hives, stomach cramps, and anaphylaxis-are well known, but the real story continues after the immediate reaction subsides.
Year‑Round Allergies: Not Just Spring
Most people think of allergies as a springtime nuisance, but year‑round allergies include reactions to indoor allergens like dust mites, pet dander, mold spores, and even certain foods that keep the immune system activated. The symptoms-runny nose, itchy eyes, congestion-can appear any month, often worsening after a food trigger.
How Food Allergies Keep Your Immune System Primed
The immune system doesn’t hit the reset button after a food exposure. When IgE antibodies latch onto mast cells, they leave the cells in a sensitized state. Subsequent exposure to an unrelated allergen-say, pollen-can cause the already‑primed mast cells to overreact, releasing more histamine than they would otherwise. This phenomenon is called cross‑reactivity where an antibody triggered by one allergen also recognizes a similar protein in another allergen.
Cross‑Reactivity: The Sneaky Bridge Between Foods and Pollen
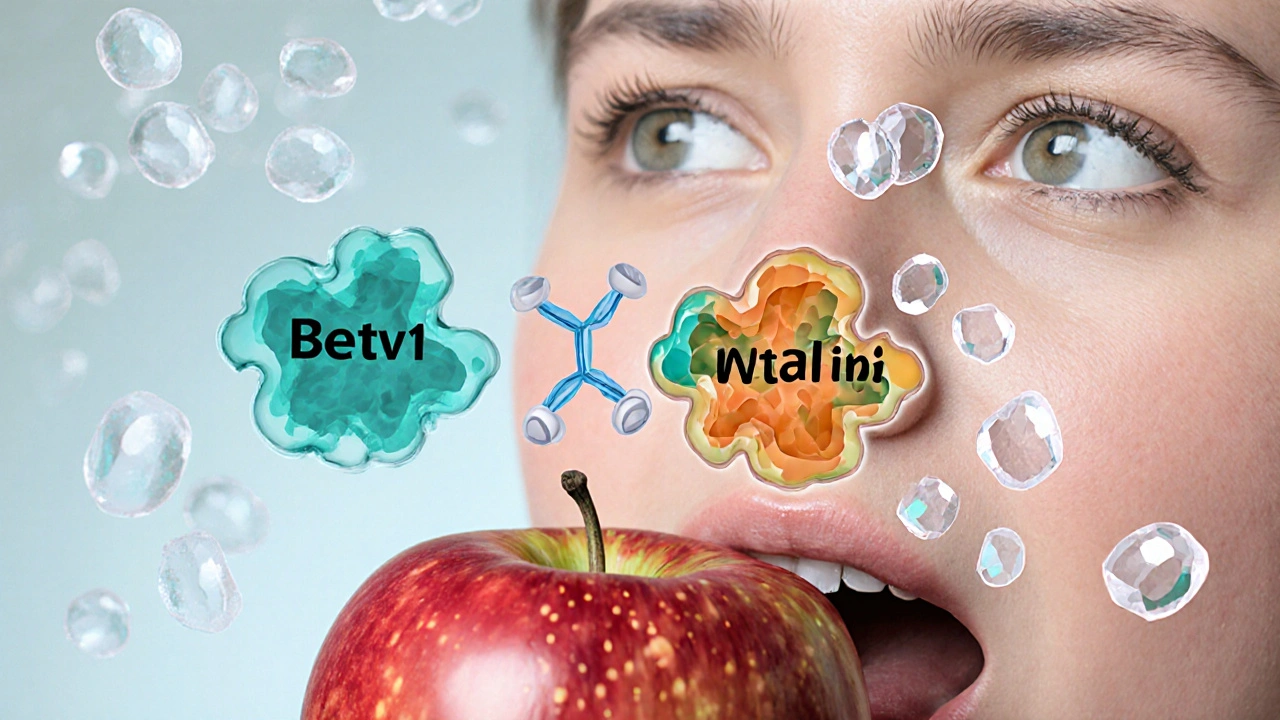
A classic example is Oral Allergy Syndrome (OAS) a condition where people allergic to pollen react to raw fruits, vegetables, or nuts that share similar proteins. Birch pollen sufferers often experience itching or swelling after eating apples, carrots, or hazelnuts. The proteins Bet v 1 (from birch) and Mal d 1 (from apple) are structurally similar, so the IgE antibodies can’t tell the difference.
Gut Health, Barrier Function, and Allergic Overlap
Recent research points to the gut microbiome the community of bacteria living in the intestines that influences immune regulation as a key player. An imbalance-known as dysbiosis-can weaken the gut lining, allowing food proteins to cross into the bloodstream more easily, priming the IgE response. A leaky gut can also release inflammatory signals that aggravate nasal passages, making you more reactive to dust mites or pet dander.
Comparing Food vs. Seasonal Allergy Triggers
| Aspect | Food Allergy | Seasonal/Year‑Round Allergy |
|---|---|---|
| Typical Triggers | Peanuts, shellfish, milk, eggs, soy | Pollen, dust mites, pet dander, mold spores |
| Onset Time | Minutes to 2hours after eating | Hours after exposure; can persist all day |
| Key Symptoms | Hives, swelling, vomiting, anaphylaxis | Runny nose, itchy eyes, sneezing, asthma flare‑up |
| Diagnostic Test | Specific IgE blood test or skin prick | Allergen‑specific IgE or nasal challenge |
| Cross‑reactivity | Often with related plant foods (OAS) | Less common, but can occur with molds and foods |
Practical Steps to Break the Cycle
- Identify all triggers. Keep a daily log of foods eaten and any allergy symptoms that follow, including nasal or eye irritation.
- Get tested for specific IgE antibodies to see which foods and inhalants share sensitization. This helps pinpoint cross‑reactive pairs.
- Work with an allergist to develop a combined management plan that addresses both diet and environmental control. It may include antihistamines, nasal sprays, or sub‑lingual immunotherapy.
- Improve gut health: incorporate probiotic‑rich foods (yogurt, kefir) and prebiotic fiber (onion, garlic) to support a balanced microbiome.
- Reduce indoor allergen load: use HEPA filters, wash bedding in hot water weekly, and keep humidity below 50% to limit dust mites and mold.
- Consider elimination diets under medical supervision to confirm which foods are truly problematic.
When to Seek Professional Help
If you notice that a mild food reaction is followed by persistent sneezing, watery eyes, or asthma symptoms that last beyond a few hours, schedule an appointment with an allergist. Early intervention can prevent escalation to chronic sinusitis or severe asthma attacks.
Future Directions: Integrated Allergy Care
Researchers are exploring biologic therapies (e.g., anti‑IgE monoclonal antibodies) that can dampen both food and environmental responses simultaneously. Early trials show promise in reducing the need for multiple medications and improving quality of life for people with overlapping allergies.
Frequently Asked Questions
Can a food allergy cause a cold‑like symptom?
Yes. When a food triggers IgE release, histamine can affect nasal passages, leading to a runny nose or post‑nasal drip that feels like a cold.
What is the difference between food allergy and food intolerance?
Food allergy involves the immune system (IgE antibodies) and can cause life‑threatening reactions. Food intolerance is a non‑immune response, often digestive, and doesn’t involve antibodies.
Why do some people develop new allergies as adults?
Changes in gut microbiota, repeated low‑dose exposures, or hormonal shifts can alter immune tolerance, leading to new sensitizations later in life.
Is it safe to eat cooked versions of foods that cause oral allergy syndrome?
Cooking often destroys the proteins that trigger OAS, so many people can tolerate the cooked form without symptoms. Always test in small amounts first.
Can allergy shots help with food‑related year‑round symptoms?
Immunotherapy primarily targets inhalant allergens, but it can reduce overall mast‑cell sensitivity, indirectly lessening the impact of food‑triggered histamine release.






Emily Torbert October 13, 2025
This stuff really hits home for anyone dealing with sneaky food triggers.
Rashi Shetty October 24, 2025
While the article correctly outlines cross‑reactivity, it omits a thorough discussion on the prevalence of self‑medication with over‑the‑counter antihistamines, which can mask underlying issues. Moreover, the guidance on integrating gut‑health strategies lacks concrete dietary references that clinicians could readily recommend 😐.
Queen Flipcharts November 4, 2025
One might argue that the immune system mirrors the collective psyche of a nation, reacting fiercely to foreign antigens as it does to external cultural influences. Thus, understanding food‑allergy cross‑reactivity becomes an act of preserving the sovereign integrity of one's internal biological frontier.
Jim Butler November 15, 2025
Take charge of your allergy management by logging every bite and every sniff of pollen – consistency breeds confidence! Pair that habit with a probiotic‑rich diet and you’ll notice the histamine storms lose their punch 🚀.
Renee van Baar November 26, 2025
Understanding how food allergies can keep your immune system on high alert is the first step toward reclaiming comfort throughout the year.
When IgE antibodies latch onto mast cells, they leave a lingering sensitization that can be triggered by completely unrelated inhalants.
This phenomenon explains why a handful of raw apples after a birch season can make your eyes water for days afterward.
The research community now recognizes that the gut microbiome plays a pivotal role in modulating that sensitization.
Dysbiosis, or an unhealthy microbial balance, can erode the intestinal barrier, allowing larger food proteins to slip into circulation.
Once those proteins circulate, they act as messengers that amplify mast‑cell activity in the nasal passages.
Practically, this means that a seemingly innocuous snack can set off a cascade that worsens your indoor dust‑mite symptoms.
To break this cycle, start by keeping a detailed diary of foods, symptoms, and environmental exposures.
Bring that diary to your allergist; specific IgE panels can pinpoint which foods and pollens share cross‑reactive proteins.
If you discover a pattern with birch pollen, consider cooking the offending fruits and vegetables, as heat often denatures the culprit proteins.
Complement dietary changes with a probiotic regimen that includes strains like Lactobacillus rhamnosus and Bifidobacterium longum.
These microbes have been shown in clinical trials to enhance regulatory T‑cell function, which can tone down IgE‑mediated responses.
Meanwhile, reduce indoor allergen load by using HEPA filters, washing bedding at 130 °F weekly, and maintaining humidity below 50 %.
For those with persistent symptoms, discuss sub‑lingual immunotherapy or even emerging anti‑IgE biologics with your specialist.
By integrating nutrition, environment, and targeted medical therapy, you empower your immune system to respond appropriately rather than overreact.
Mithun Paul December 7, 2025
The preceding exposition, while comprehensive, fails to address the statistical significance of the cited probiotic trials, thereby limiting its applicability to evidence‑based practice.
Sandy Martin December 18, 2025
I totally get how frustrating those hidden triggers can be – keeping a food‑symptom log really changes the game, just make sure you’re consitnt with timing.
Steve Smilie December 29, 2025
One cannot help but marvel at the article’s cursory treatment of antihistamine stewardship; a nuanced discourse would invoke pharmacodynamic subtleties rather than mere emoji‑laden caution.
Josie McManus January 9, 2026
Yo, that short line nailed it – food allergies are a silent bully that keep you on edge, so shut that noise down by knowing your triggers.
Heather Kennedy January 20, 2026
From a clinical perspective, the intersection of aeroallergen sensitization and oral allergy syndrome underscores the necessity for integrated allergen‑specific IgE profiling.
Janice Rodrigiez January 31, 2026
Think of your immune system as a symphony – when one instrument (a food protein) goes off‑key, it throws the whole orchestra into disarray, so tuning your diet can restore harmony.
Roger Cardoso February 11, 2026
Some claim these cross‑reactivity charts are purely scientific, yet one wonders who profits from the burgeoning market of proprietary allergy tests.
barry conpoes February 22, 2026
Let’s be clear: the United States leads in allergy research, and adopting these protocols is a patriotic duty to safeguard our citizens’ health.
Kristen Holcomb March 5, 2026
Great deep dive! I’m curious, have you seen any data on how seasonal shifts in pollen counts specifically alter gut permeability?
justin davis March 16, 2026
Wow!!! That metaphor is sooo vivid-just what we needed to imagine immune chaos while eating a strawberry!!! 🍓
David Lance Saxon Jr. March 27, 2026
One could argue that the article’s omission of pharmacokinetic considerations reflects a broader epistemic complacency within the field, prompting a re‑evaluation of our diagnostic heuristics.
bruce hain April 7, 2026
While the piece is informative, its practical recommendations are overly generic and lack actionable specificity.